Anxiety and Panic Disorders in Canada: Symptoms, Causes, and Why Rates are Rising
Is anxiety becoming more common in Canada? Recent data suggests a resounding yes. Currently, one in four Canadians will meet the criteria for an anxiety disorder in their lifetime, making them the most prevalent mental illnesses in the country.
Since 2012, cases of Generalized Anxiety Disorder (GAD) have doubled. Understanding the difference between chronic worry and the acute physical intensity of Panic Disorder is essential for those seeking effective treatment as diagnosis rates continue to climb across Canada.
Why is Anxiety Rising in Canada? Understanding the 2024 Statistics
Anxiety disorders are responsible for considerable disability and negatively impact a person’s ability to function in work, school, and social settings. The rapid increase in diagnoses, particularly since 2012, is a call to action.
Generalized Anxiety Disorder (GAD) Doubled: The 12-month prevalence of Generalized Anxiety Disorder (GAD) among Canadians aged 15 and older doubled from 2.6% in 2012 to 5.2% in 2022 (Statistics Canada, 2023).
The Youth and Gender Crisis: The rise in anxiety is most pronounced among youth and young women. Young women aged 15 to 24 experienced the steepest increase in GAD, with rates nearly tripling (from 3.8% to 11.9%) between 2012 and 2022 (Statistics Canada, 2023). Overall, women are consistently about twice as likely as men to be diagnosed with a mood or anxiety disorder in Canada.
Specific Prevalence: Among the various types of anxiety, GAD is particularly common, with an estimated 13.3% of people experiencing it in their lifetime. Panic Disorder, characterized by recurrent, unexpected panic attacks, has a lifetime prevalence of around 3.7% (Public Health Agency of Canada, 2016).
The Social Media Feedback Loop: Anxiety in Youth
The dramatic rise in anxiety among adolescents and young women is strongly linked to the ubiquity of social media. Research indicates that the time spent on these platforms is a significant predictor of mental distress, especially among girls, whose GAD rates have tripled.
The Mechanisms Driving Distress
Upwards Social Comparison
Platforms like Instagram and TikTok expose users to curated, highly unrealistic versions of their peers' lives, leading to constant and often damaging upward social comparison. This encourages feelings of inadequacy, low self-esteem, and social anxiety.
Fear of Missing Out (FOMO)
The perpetual availability of social interaction creates intense pressure to remain constantly engaged. FOMO drives compulsive checking behaviour, disrupts sleep, and keeps the brain in a perpetual state of hyper-arousal, contributing directly to chronic anxiety.
Cyberbullying and Digital Harassment
Social media is a major vector for harassment. For young people, particularly girls, exposure to cyberbullying significantly increases the risk of developing anxiety and depressive symptoms, often resulting in avoidant behaviours that mirror phobias.
Sleep Deprivation
Using devices late at night inhibits the production of melatonin (the sleep hormone), leading to chronic sleep deprivation. Sleep loss severely impairs the brain's ability to regulate mood and emotion, making the Amygdala (the brain's fear centre) more reactive and making generalized anxiety worse.
Beyond Palpitations: The Full Spectrum of Panic Attack Symptoms
A hallmark of a panic disorder is the sudden, intense panic attack, which involves a terrifying surge of discomfort that peaks within minutes. The experience is often so visceral that it mimics a medical emergency, leading many sufferers to believe they are having a heart attack or stroke.
Physical Symptoms (Fight-or-Flight Response)
The primary symptoms are directly linked to the activation of the sympathetic nervous system (the "fight-or-flight" response) and include:
Cardiovascular: Racing heart (palpitations), pounding heart, or an accelerated heart rate; chest pain or discomfort.
Respiratory: Sensations of shortness of breath, smothering, or choking.
Body: Sweating, trembling, or shaking; dizziness, unsteadiness, or feeling faint.
Psychological: An overwhelming fear of losing control, "going crazy," or dying.
Extreme and Dissociative Symptoms
The panic response is highly variable and can lead to complex neurological and sensory symptoms that are often missed in mainstream descriptions. These symptoms occur because hyperventilation and extreme adrenaline cause blood vessel constriction (vasoconstriction), reducing blood flow to the extremities and the brain's non-essential areas:
Paresthesia and Numbness: Tingling, prickling, or intense numbness (known as paresthesia) in the hands, feet, face, and head, which can lead to the severe feeling of an oncoming stroke or neurological crisis.
Vision Loss/Disturbances: Temporary changes in vision, such as blurriness, tunnel vision, or momentary vision loss (lasting seconds to a minute). This can be triggered by extreme changes in blood pressure, adrenaline, or anxiety-induced migraine.
Derealization and Depersonalization: A profound, frightening sense of detachment from reality (derealization) or feeling detached from one's own body (depersonalization). These dissociative symptoms are terrifying and contribute to the fear of "losing control".
The Critical Difference: GAD vs. Panic Disorder
While both disorders involve anxiety, they differ fundamentally in focus, intensity, and duration. Misdiagnosis often occurs when the two are conflated.
Generalized Anxiety Disorder (GAD)
Nature of Worry: Chronic, persistent, and diffuse ("free-floating").
Focus of Worry: Everyday, realistic concerns such as health, money, family, or job performance.
Intensity: Moderate-to-high, characterized by a constant state of tension, but usually manageable.
Somatic Symptoms: Muscle tension, fatigue, irritability, and insomnia (chronic physical strain).
Onset: Gradual, often starting in childhood or adolescence.
Panic Disorder
Nature of Worry: Episodic, acute, and intense.
Focus of Worry: Primary focus is on the next panic attack and the physical consequences (dying, going crazy).
Intensity: Extreme, debilitating, peaking suddenly and dramatically.
Somatic Symptoms: Cardiovascular and respiratory distress (sudden, terrifying physical cascade).
Onset: Abrupt, often starting in late adolescence or early adulthood.
Key Takeaway: A person with GAD worries constantly about future problems (e.g., losing their job). A person with Panic Disorder is primarily worried about the imminent physical symptoms of having another panic attack.
The Neurobiological Mechanism: Why Panic Feels Like a Physical Threat
Anxiety disorders, like Substance Use Disorder, are rooted in complex neurobiology. The main biological driver is the Amygdala, the brain's central fear-processing hub.
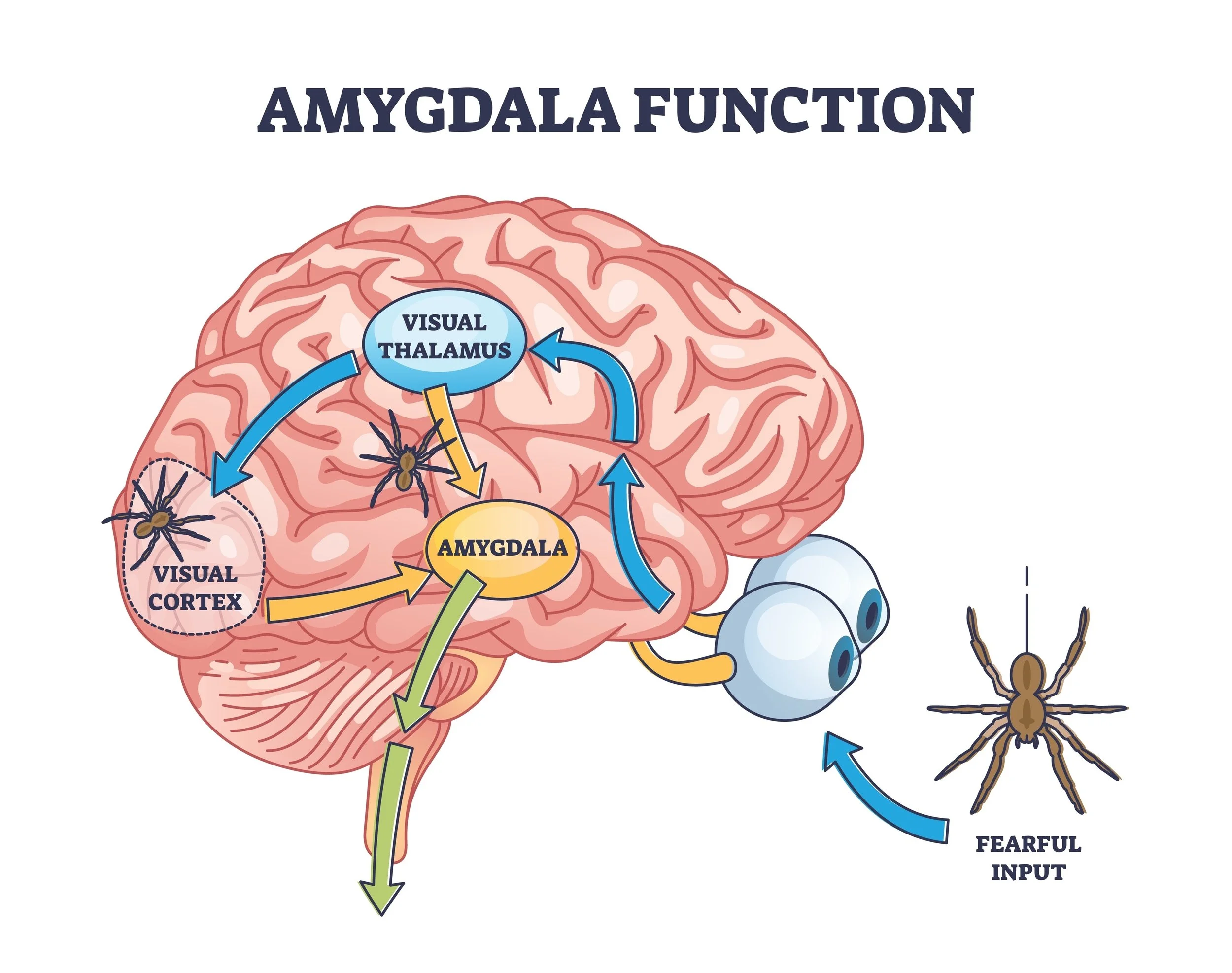
The Amygdala's Role
The Amygdala acts like a smoke detector. In people with anxiety disorders, this alarm system is often set to an over-sensitive frequency. It can be triggered by real external threats or internal signals, such as a slight increase in heart rate.
Image depicting the function of the amygdala and the fear response
Interoception: The Body's Internal Alarm
A key factor that distinguishes panic disorder is a phenomenon known as Interoception: the sense of the internal physiological condition of the body.
People with panic disorder often display heightened interoceptive attention—they are excessively focused on internal body signals (like heartbeats, breathing rate, or stomach tension).
When a benign sensation occurs (e.g., a natural quickening of the heart from climbing stairs), the hyper-vigilant Amygdala is triggered. The person then catastrophically misinterprets this signal (e.g., "My heart is racing; I must be dying").
This catastrophic belief unleashes the massive, physical panic attack, completing the self-fulfilling cycle where the initial harmless bodily signal (interoceptive cue) creates the full-blown, terrifying physical experience of panic.
Evidence-Based Pharmacotherapy: The Role of SSRIs
While psychotherapy, particularly CBT, is essential, Medication-Assisted Treatment (MAT) is often required to stabilize brain chemistry and provide relief, especially for severe or chronic GAD and Panic Disorder.
Selective Serotonin Reuptake Inhibitors (SSRIs)
SSRIs are the first-line pharmaceutical treatment for most anxiety disorders due to their strong efficacy and safety profile.
Mechanism of Action: SSRIs work by increasing the concentration of the neurotransmitter serotonin in the synaptic gap of the brain. Serotonin is often called the "feel-good" or "modulator" chemical.
The Desensitization Effect: Through the gentle but persistent increase of serotonin levels, SSRIs help to desensitize the over-reactive Amygdala over several weeks. This dampens the intensity of the "alarm signals," reducing both the chronic, anticipatory worry of GAD and the severity of panic attacks.
Common Examples: Citalopram (Celexa), Sertraline (Zoloft), and Escitalopram (Lexapro). It is crucial for patients to understand that full therapeutic effect may take 4 to 8 weeks, and treatment is a long-term strategy, not a quick fix.
Short-Term Relief: Benzodiazepines
In emergency or severe crisis situations, fast-acting medications like benzodiazepines (e.g., Ativan, Xanax) may be used. However, due to the high risk of dependence and withdrawal severity, these are typically reserved for short-term use during treatment initiation or as a rescue medication for acute panic attacks.
The Systemic Barrier: Cost and The Access Crisis
Despite the severity and widespread nature of these conditions, a major systemic challenge remains the lack of equitable access to care.
Unmet Needs: Data shows that more than one-third (36.6%) of Canadians who met the criteria for a mood or anxiety disorder reported unmet or partially met health and mental health care needs in 2022.
The Cost of Effective Treatment: The cost of services is frequently cited as a significant obstacle to receiving effective, evidence-based treatments like Cognitive Behavioural Therapy (CBT). While CBT has proven to be clinically and economically effective in global studies, publicly funded CBT is scarce in Canada, creating a massive inequity in service delivery. This means Canadians are often forced to pay for private psychology and psychotherapy, which can cost hundreds of dollars per session, a barrier that disproportionately impacts low-income and vulnerable populations.
Economic and Social Determinants
Similar to the SUD crisis, economic factors are exacerbating anxiety. Canadians report that their mental health has been negatively impacted by the economic downturn, with 1 in 3 Canadian households experiencing difficulties meeting their financial needs for necessary expenses like housing and food. High rates of food and housing insecurity are directly tied to high levels of anxiety, demonstrating that social determinants of health are not just abstract concepts—they are powerful drivers of mental illness.
Conclusion: The Path to Comprehensive Care
Anxiety and panic disorders in Canada are an escalating crisis rooted in a complex interplay of neurobiological vulnerability, environmental stressors (like social media), and a systemic failure to provide accessible, evidence-based care. Addressing this requires a commitment to:
Universal Access: Establishing publicly funded, easily accessible psychological services, particularly CBT, to ensure treatment is a right, not a privilege.
Integrated Treatment: Implementing models that combine pharmacotherapy (SSRIs) for biological stabilization with therapeutic intervention (CBT) to teach coping skills and reframe anxious thoughts.
Targeted Support & Digital Wellness: Acknowledging the extreme and often neurological presentation of panic attacks, ensuring that medical professionals are trained to correctly diagnose anxiety and rule out medical causes, while actively promoting digital wellness and sleep hygiene for youth.
Understanding the Treatment Options
For those seeking relief, understanding which specific evidence-based treatment—such as Cognitive Behavioural Therapy (CBT), Acceptance and Commitment Therapy (ACT), and pharmacotherapy—is the gold standard for managing anxiety and panic disorders is the critical next step.
Anxiety & Panic FAQ
Yes. Extreme anxiety triggers a massive adrenaline surge and hyperventilation, which can cause blood vessels to constrict. This often results in paresthesia (numbness/tingling) in the face or limbs, tunnel vision, and a frightening sense of detachment from reality.
SSRIs work by increasing serotonin levels in the brain, which helps desensitize an over-reactive Amygdala (the brain's fear center). Over several weeks, this lowers the frequency and intensity of "false alarms," making it easier to manage both GAD and panic triggers.
Generalized Anxiety Disorder (GAD) involves chronic, persistent worry about everyday life concerns. Panic Disorder is episodic and intense, where the primary fear is the physical symptoms of the panic attack itself and the fear of when the next one will happen.
Research points to a "social media feedback loop" involving upward social comparison, cyberbullying, and sleep deprivation. These digital stressors keep the adolescent brain in a state of hyper-arousal, contributing to GAD rates doubling in the last decade.